Many diagnostic tests for COVID-19 disease are available at this time. In this blog post, we are going to focus on showing the characteristics and the main advantages to be used in the detection, screening and monitoring of the disease.
Introduction
A range of molecular techniques are being developed, ranging from laboratory tests for the diagnosis and management of COVID-19 patients to tests you can do at home. These techniques, while well known to researchers and clinicians, as well as antibody and antigen assays, may be relatively unknown to the general community. This blog post has been written to describe and explain the basic principles of the main diagnostic tests for COVID-19 currently in use.
Reverse transcription and polymerase chain reaction (RT-PCR)
PCR is a very common technique that has been (and is) used in research and diagnostics for the last 30 years to detect genetic information. RT-PCR is a version of this technique to detect the presence of RNA. This technique is currently being used as a test to detect the presence of the SARS-CoV-2 virus. This type of test has often been used as a first-line test for COVID-19, as it directly tests for the presence of the virus’s RNA.
RT-PCR tests are quite fast, sensitive and reliable, capable of producing results in 3-4 hours, although this usually takes longer if the samples must first be sent to specialized external laboratories (6-8 hours on average). Many diagnostic and research companies produce RT-PCR products, tests, and machines to make the technology widely available. Some RT-PCR tests are developed as an “all-in-one” kit, reducing laboratory handling and the potential for contamination.
How does it work?
Once the sample is collected, proteins and other molecules must be removed, isolating only the RNA. This will be a mixture of a person’s genetic material, as well as any viral RNA that may be present.

The enzymes in the kit transcribe RNA into DNA, which is amplified to allow virus detection using a thermocycler that generates a temperature program to produce approximately 35 billion copies of viral DNA for each strand of viral RNA found. was originally present. Fluorescent markers are used that are capable of binding to the amplified DNA and producing light, which can be read by the machine to produce the test result.
If the intensity of the produced light reaches a certain threshold, it is classified as a positive result. The number of PCR temperature cycles required before reaching the fluorescence threshold is recorded and provides an estimate of the amount of virus present in the patient sample. First, the viral DNA is heated to 94°C, separating the two DNA strands. Immediately afterwards, the reaction is cooled to 55ºC. This fact allows small portions of complementary DNA (primers) to bind to the viral DNA.

Finally, the temperature is raised to 72°C so that the Taq polymerase can elongate each of these DNA strands. And in this way, a new PCR cycle begins.
What does the RT-PCR test detect?

RT-PCR detects whether or not viral RNA is present in a patient’s samples. It does this by amplifying regions of the virus’s genetic material, usually the spike protein, the N protein, or the virus envelope. The RT-PCR result indicates the number of cycles necessary to detect a DNA detection threshold, in such a way that the more virus present in the sample, the fewer cycles necessary to obtain the signal. Commonly, these samples are taken from the nose or throat using long or short swabs.
What does the result obtained mean?
An RT-PCR test is highly sensitive and its result provides information about whether the virus is present in the patient.
- Positive test result: A positive PCR result means that the person from whom the sample was taken is currently infected with the virus.
- Negative test result: A negative PCR result could mean that: the person is not currently infected by this virus, or that the virus is not present in the place where the sample was taken, also a false negative could be the result of a low quality sample or, that is it too soon or too late in infection to detect virus replication. This is why negative test results require new patient samples to be taken a few days later to reduce the chance of incorrectly missing an infected person.
The RT-PCR test cannot detect if a person has had the virus and has overcome the COVID-19 disease, since it only detects when the virus is active.
Advantage:
- RT-PCR is a robust technique.
- Since RT-PCR is so common in laboratories, the technology is already in place to detect the presence of the virus.
- RT-PCR can detect ongoing infections, allowing medical personnel to determine who is currently infected and who is not.
Limitations:
- RT-PCR is based on the detection of the virus, so for counting purposes, it is possible to miss those patients who have cleared the virus and recovered from the disease.
- The distribution of the virus through the respiratory tract varies between patients, so even if a person is infected, the virus is sometimes only detectable in sputum or nasopharyngeal swab, but not necessarily in both places at the same time.
- The RT-PCR for COVID-19 can only determine if a person is currently infected with this particular coronavirus. You cannot provide information about other illnesses or symptoms.
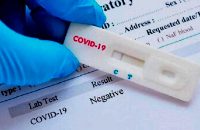
Lateral Flow / Colloidal Immunochromatography

Immunochromatographic lateral flow assays have been commonly referred to as “Rapid Tests” in the media, as they are currently used to detect antibodies to disease in a patient’s blood. Lateral flow tests can detect antibodies to the virus in a patient’s blood, indicating that the patient has COVID-19 or has recovered from COVID-19.
Lateral flow antibody tests for SARS-CoV-2 must be prescribed and used by healthcare personnel. They require a drop of the patient’s blood, usually from a finger prick, similar to tests to check blood sugar in certain types of diabetes. These tests work very differently from the RT-PCR technique and focus on detecting the patient’s immune response to the virus rather than detecting the virus itself.
How does it work?
Lateral flow immunoassays are simple devices that can detect antibodies in the blood. Healthcare personnel take a small blood sample from the patient and drop it on a sponge inside the device. A few drops of buffer are then added to help the blood sample flow through the device. As the sample moves through the device, the antibodies to SARS-CoV-2 that are present in the sample will capture the antibodies in the test and control lines. This capture and binding process produces a color change along the test and control lines that can be seen with the naked eye, producing one, two, or three lines depending on the type of antibodies present (IgM or IgG).

What does the lateral flow test detect?
Lateral flow immunoassays for SARS-CoV-2 detect two types of protective antibodies that are produced by the body when the immune system is activated. These antibodies help fight disease and remain in the blood for months after the virus and disease are cleared. The presence of antibodies in the body is often called immunity or that a person is immune to a virus, since these antibodies protect against reinfection and the return of the same disease.
When we are infected with a virus, our immune system produces early IgM antibodies with intermediate strength binding to the virus, which can start working to clear the virus about 5 days after a new infection. Usually, 8 to 10 days after infection, IgG antibodies with high binding strength can help clear the virus more quickly. Antibody lateral flow immunoassays can be designed to detect IgM or IgG alone or both together.
What does the result obtained mean?
Lateral flow antibody immunoassays detect antibodies to the virus in the blood. They do not detect the virus itself. Antibody tests provide an enormously important ability to detect past infection with viruses to identify people who were asymptomatic, people who have cleared the virus and are therefore no longer at risk of becoming infected or transmitting the virus to other people In addition, antibody tests are critical to assess the spread of the virus to the population and the level of “herd” immunity in the population. This is important to understand the potential consequences of lifting or enforcing measures to control the virus, such as quarantine, social distancing, school and workplace closures.

Lateral flow immunoassay tests to assess for the presence of IgG and IgM antibodies are very simple to interpret: A control line should appear to show that the assay has worked correctly. Other results that may appear are some of the types of antibodies found in the sample. The appearance of lines for IgG or IgM, or both, indicates a positive sample and therefore, that the patient has been infected with the COVID-19 coronavirus.
Advantage:
- Lateral flow assays are extremely fast, providing results in just 15 minutes.
- They allow non-invasive sampling to detect the presence of the virus.
Limitations:
- Accuracy in diagnosing coronavirus is limited.
- Until now, available lateral flow kits can only determine if a patient has ever been infected with COVID-19. More tests would be needed to verify if a patient is currently infected.
ELISA type immunoassays
An ELISA is a common technique that can be used to detect antigens or antibodies. An ELISA is a common technique that can be used to detect antigens or antibodies. The strength of the color change is proportional to the number of antibodies present in the sample. ELISAs allow up to 96 assays to be completed at the same time, providing an economical and effective method for testing batches of many samples at the same time. This technology could help speed up the number of patients that can be tested for SARS-CoV-2.
How does it work?
An ELISA detects antibodies produced in the patient’s blood due to infection with SARS-CoV-2. The entire experiment can be performed in one well and involves mixing patient samples, antibodies, antigens, and enzymes together with a substrate that, when metabolized, turns into a color-changing product. Let’s look at the following diagram:

- A plasma sample from the patient is added to the well containing the SARS-CoV-2 specific antigen.
- The antibodies present (or not) against SARS-CoV-2 in the patient’s plasma bind to the antigens arranged at the bottom of the well, the rest of the elements present in the plasma sample are eliminated by washing.
- Enzyme-linked secondary antibodies are added and bind to the patient’s antibodies. Excess antibody not bound to the patient’s antibody is washed away.
- The substrate that is recognized by the enzymes that are bound to the secondary antibody is added.
- In the wells that the antibodies against SARS-CoV-2 are found, they begin to change color.
- The product formed is capable of being objectively determined with a plate reader.
- If the patient was not infected with COVID-19, the whole process cannot be carried out, so that a color change does not form in the well.
What does the ELISA test detect?
Antibody ELISA kits are detecting the antibody response to COVID-19 infection. Detection of antibodies to SARS-CoV-2 could tell a clinician if a patient has been infected with COVID-19, either currently or in the past. However, infected patients will not be detected immediately after infection, but only when the immune system to the virus can be detected in the blood, approximately 5 days after infection. Current knowledge suggests that once a person has been infected with the virus, their immune system will prevent future infection with the same virus.
The ELISA kit for the presence of antibodies provides very important information for the diagnosis, management and recovery of COVID-19 and also helps researchers to assess how many people in the population have been infected, which is important for planning the infection control.
What does the result obtained mean?
An ELISA kit shows a positive result (well color change) if the patient has antibodies to SARS-CoV-2. This might not mean that they currently have the virus, just that they have had it at some point. This is because the antibodies remain in the blood even after the infection clears up. A negative result would mean that the patient has not been infected with COVID-19 and may not have immunity against it.
Advantage:
- ELISA is a simple and cheap laboratory technique.
- ELISAs are well established and documented assays within the scientific and medical community.
- Results can generally be generated within 1 to 3 hours of sample collection from the patient.
- ELISA kits allow testing many patients at once.
Limitations:
- They cannot be carried out in situ, the samples must be collected, processed and analyzed in a laboratory.
Conclusions
- Three main types of tests are being used or developed to detect SARS-CoV-2.
- These diagnostic tests are in different stages of development, validation and production.
- Each type of assay has its own advantages and disadvantages inherent to the underlying technology.
- A combination of test types used at different times may be useful for patient management and population pandemic control.
| Technology | Molecule tested | Requirements | Time required | Type of sample | Number of samples |
| RT-PCR | Viral RNA | Laboratory | 3-4 hours | nasopharyngeal swab or sputum | Up to 96 samples |
| Lateral Flow | IgG and IgM antibodies against SARS-CoV-2 | Assistance point | 15-20 minuts | Blood | 1 sample per test |
| ELISA | IgG and IgM antibodies against SARS-CoV-2 | Laboratory | 1-3 hours | Blood | Up to 96 samples |
If you need more information or have any questions, do not hesitate to ask us:




14 comments on “Types of tests to detect COVID-19”
Eli Richardson
It really helped when you mentioned how PCR tests detect how many antibodies our body’s making to protect us. My best friend is getting married soon and asked his guests to get tested before the wedding date. My wife and I want to know which test would be better for us, so we’ll keep reading your article. Thank you for helping us understand how an antibody test works to identify the virus in our blood.
pcr test
Such a great information. This is really very helpful for bloggers
pcr test
You’re doing a great job Man, Keep it up.
home PCR
You’re doing a great job Man, Keep it up.
rt pcr
Usually I never comment on blogs but your article is so convincing that I never stop myself to say something about it. Really helpful.
Mobeen
All test failed to detect Covid-19, but somehow it helps to detect the right one but not accurate.
thetradebuzz
Thetradebuzz is a leading B2B marketplace where you can interact with global manufacturers, suppliers, buyers, and importers to conduct business online.
The Business Witness
The Business Witness gives latest updates and articles about business and marketing, technology, sports and games, as well as travel and tourism guides.
Write For Us
The Inforinn is one of the greatest blog websites that provide updated and useful information for blog readers and here you can Write For Us for all topics
Marketing Tips & Tricks
Fantastic article. Your works are distinctive, easy to understand, and contain informative and inspiring material. Keep up the fantastic work!
Travel Guides and Tips
You are awesome. Such an informative post about world worrier to increase my knowledge. Thanks for posting this and keep sharing buddy.
Visit us : Travel Guides and Tips
Adobe Photoshop Serial Number
This blog post is absolutely fantastic! The content is insightful and well-researched, and your writing style is engaging and easy to follow. I love how you provide practical tips that can be applied right away. Keep up the great work!
Arturia Pigments VST Crack
This informative article a very good approach toward data you provide good work. May all your dreams come true and may you find happiness and success in all your endeavors. Best wishes to you always.
Line 6 Helix Native Crack
I am happy to find this article content very helpful and valuable for everyone, as it contains lot of topic information.